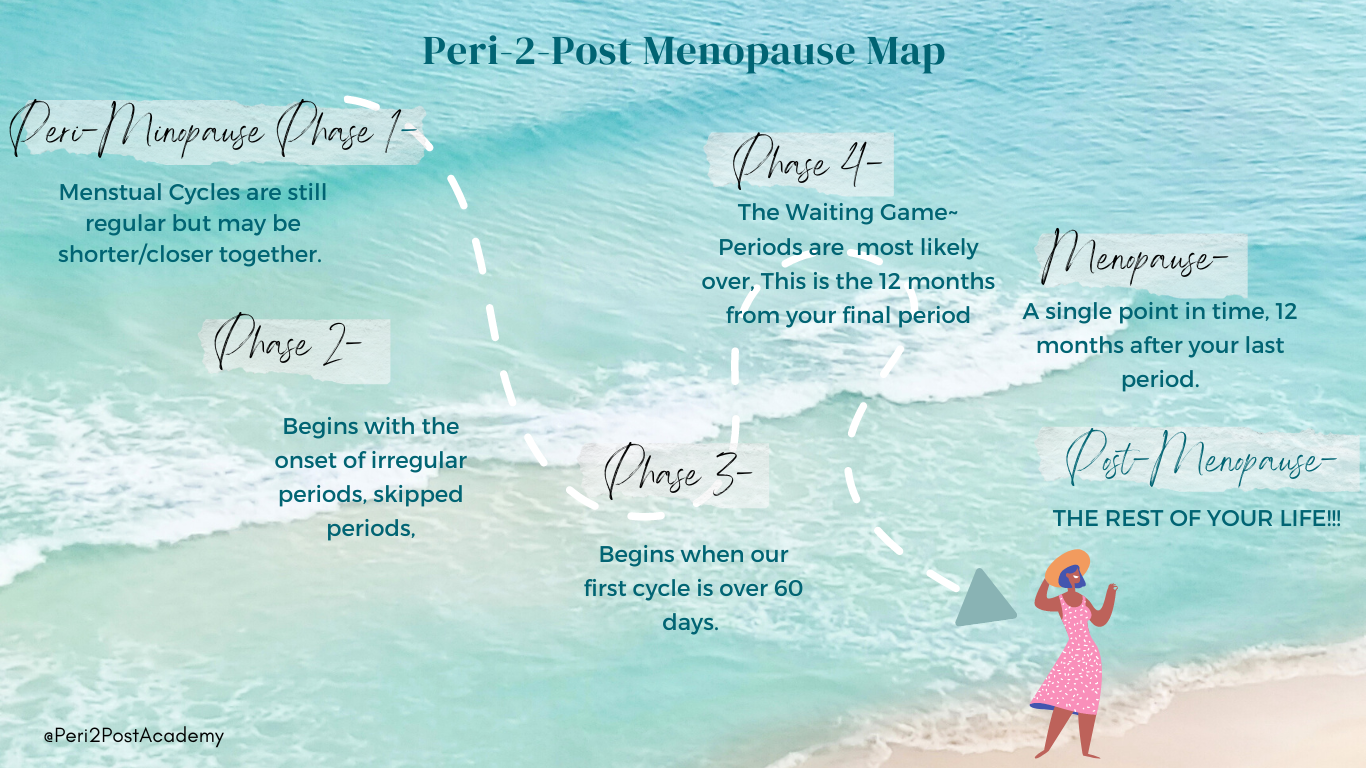
Our genetics, life history, and lifestyle all influence when and how we experience the Peri-2-Post Transition. However, there are some general patterns that women go through if this transition occurs naturally (not medically induced). And, just as our experiences are unique, the solutions that work best for each of us are also unique.
Typically, Perimenopause transition is divided into two stages: the early stage and the late stage. Hormone levels fluctuate during the early stage, and estrogen production decreases during the late stage. Looking at it from a biochemical/hormonal perspective, I see there is a clear breakdown of Perimenopause into 4 Phases. Each phase is linked to specific symptoms that may arise due to these biochemical changes. Let’s delve deeper into this transition…
Peri-2-Post Phase 1
Early Perimenopause and Low Progesterone: The First Signs to Recognize
Early perimenopause often begins with declining progesterone, even while menstrual cycles still appear regular.
Many women in their late 30s and 40s experience anxiety, sleep disruption, heavier bleeding, or mood changes before realizing ovulation has become inconsistent.
This first phase of perimenopause is subtle.
But it is not random.


Peri-2-Post Phase 2
Early Perimenopause Stage 2: Fluctuating Estrogen and Irregular Cycles
The second stage of perimenopause is defined by cycle irregularity and pronounced estrogen fluctuation.
During this phase, menstrual cycles may vary by more than 6–7 days in length. Ovulation becomes inconsistent, progesterone remains low, and estrogen levels may swing higher — and lower — than before.
This is not steady decline.
It is volatility.
And volatility creates symptoms.
Peri-2-Post Phase 3
Stage 3 Perimenopause: When Estrogen Truly Declines
Stage 3 perimenopause begins when cycles become widely irregular — including your first cycle longer than 60 days.
This stage marks a shift from hormonal volatility to overall hormonal decline.
While estrogen may still fluctuate occasionally, the dominant pattern becomes:
Low progesterone
Low estrogen
Irregular or absent ovulation
Symptoms begin to reflect sustained estrogen withdrawal rather than dramatic swings.


Peri-2-Post Phase 4
Stage 4 Perimenopause: The Transition to Menopause
August 7, 2024
Stage 4 perimenopause is marked by increasingly infrequent menstrual cycles — sometimes nearing cessation — but not yet reaching the full 12 consecutive months required to define menopause.
Ovulation has largely stopped.
Estrogen levels are now consistently low.
The hormonal volatility of earlier stages settles — but sustained estrogen deficiency introduces a new pattern of symptoms.
Menopause
Menopause is commonly defined as the point in time when a woman has gone 12 consecutive months without a menstrual period. That definition is technically correct. But it is incomplete. It centers on bleeding, not biology.
For women with hysterectomy, using Birth Control or IUD, irregular cycles, or endometrial ablation, the “12-month rule” offers little clarity.
But biologically, menopause is a gradual transition that unfolds over years, during perimenopause, and then stabilizes into a low-hormone baseline.
Menopause is both:
• A symptomatic transition
• A permanent hormonal shift
Understanding both aspects matters.